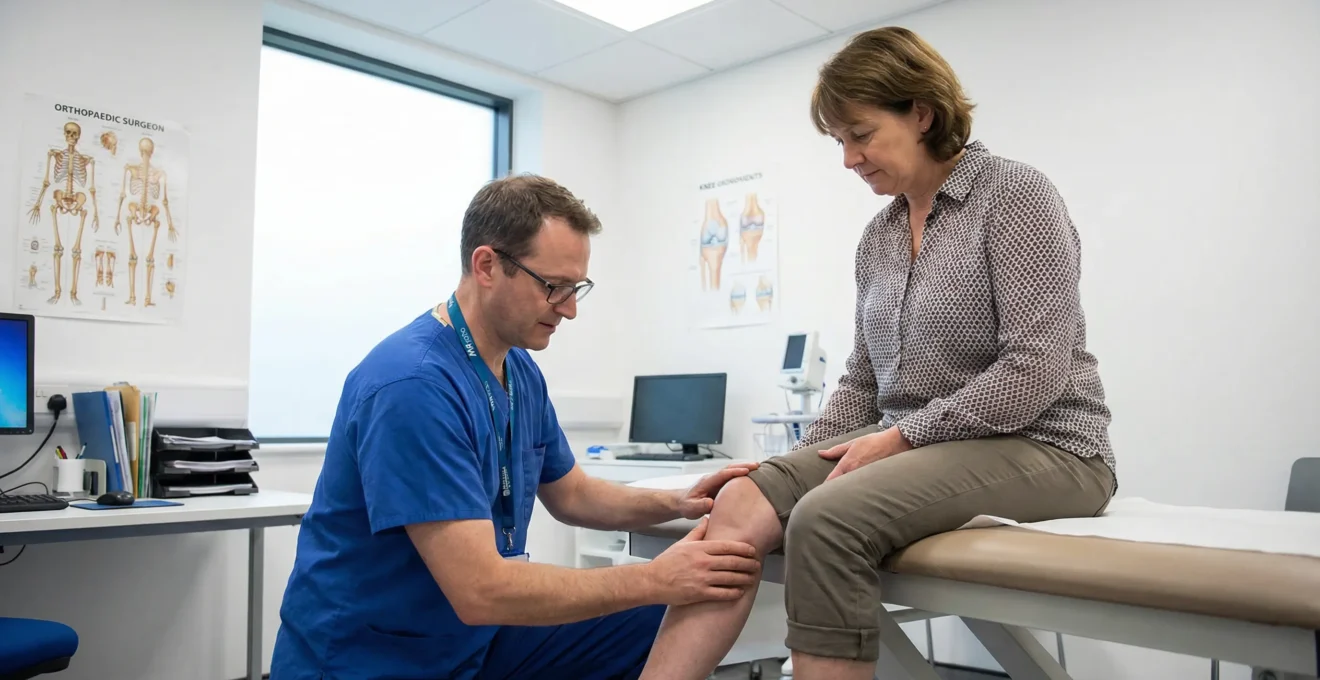
Here is what most online resources will not tell you. Surgeons do not simply look at your pain level and book you in for theatre. The decision involves a careful assessment of multiple clinical factors, each weighted differently depending on your specific situation. Understanding these factors before your consultation transforms you from a passive patient into an informed participant in your own care.
The 5 factors in 30 seconds:
- Structural damage: What imaging reveals about your joint
- Functional limitation: How much your knee affects daily life
- Conservative treatment: What you have tried and how it worked
- Overall health: Your fitness for surgery
- Expectations: Whether outcomes match your goals
Patients often assume that severe knee pain automatically makes them candidates for surgery. However, the decision is more nuanced. A qualified knee surgeon evaluates both the structural condition of the joint, as seen on imaging, and the patient’s specific symptoms. Surgery is considered appropriate only when these factors align.
The following overview is not intended as a self-diagnosis guide. Instead, it provides insight into how experienced knee surgeons assess candidacy, prioritize treatment options, and determine the best approach for each patient. Understanding this perspective allows patients to approach consultations with informed questions, engage in meaningful discussions, and make well-considered decisions about their knee care.
What you will discover
- Why Surgeons Don’t Rely on Pain Alone: The Structural Damage Assessment
- Functional Limitation: When Your Knee Stops You Living
- The Conservative Treatment Threshold: What You Must Try First
- Your Overall Health: The Surgical Risk Calculation
- Patient Expectations and Lifestyle Goals: The Often Overlooked Factor
Why Surgeons Don’t Rely on Pain Alone: The Structural Damage Assessment
One aspect that often surprises patients is this: two people with identical pain levels can receive completely different recommendations. One gets scheduled for surgery. The other gets sent home with a physiotherapy referral. The difference lies in what the imaging reveals.
MRI and X-ray findings form the foundation of any surgical candidacy assessment. Surgeons are looking for specific structural abnormalities—cartilage loss, ligament tears, meniscal damage, bone-on-bone contact. These findings must correlate with your reported symptoms. A torn ligament that is not causing instability might not require reconstruction. Severe arthritis visible on X-ray that is not significantly limiting function might not warrant replacement. The imaging tells a story, but it is only part of the narrative.
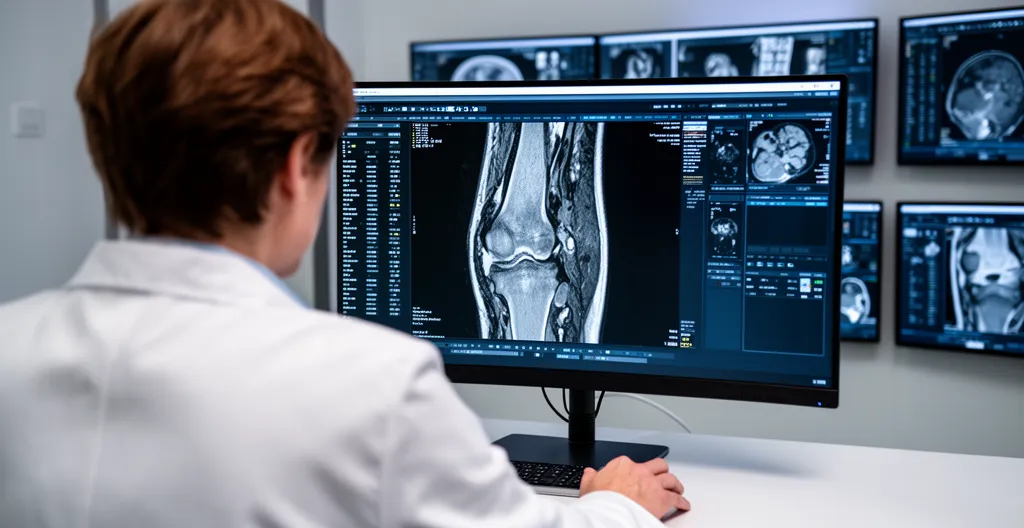
Consulting a high-volume knee surgeon with extensive experience across both sports traumatology and joint replacement ensures this correlation is properly evaluated. Surgeons performing hundreds of procedures annually develop an instinct for when imaging findings genuinely warrant intervention—and when they do not.
Surgery types, different criteria: The structural findings that justify surgery vary dramatically by procedure. ACL reconstruction typically requires documented ligament rupture plus functional instability. Knee replacement requires advanced cartilage degeneration with bone involvement. Arthroscopy might address meniscal tears causing mechanical symptoms. The same MRI can indicate surgery for one condition while ruling it out for another.
What experienced knee surgeons look for is the match between objective findings and subjective experience. I recall observing a consultation where a patient presented with an MRI showing significant cartilage wear—the kind that might alarm anyone searching their condition online. But the surgeon spent thirty minutes assessing function, asking about daily activities, testing stability. The recommendation? Not surgery. Not yet. The structural damage existed, but the functional impact did not justify the risks of intervention.
Functional Limitation: When Your Knee Stops You Living

I remember meeting Marcus, a 55-year-old warehouse supervisor, during a clinic observation. He had delayed seeking help for eighteen months, hoping his knee would sort itself out. By the time he arrived, the cartilage damage had progressed to a point where his treatment options had narrowed considerably. Earlier evaluation might have offered more possibilities.
Surgeons assess functional limitation through specific questions about your daily life. Can you walk to the shops? Climb stairs? Get in and out of a car? Sleep through the night without pain waking you? These are not casual enquiries. They form part of standardised assessment tools that quantify how severely your knee affects your quality of life.
The most common misconception I encounter is patients assuming that severe pain alone determines candidacy. Pain matters, certainly. But a surgeon needs to understand how that pain translates into functional restriction. Someone experiencing moderate pain but struggling to perform basic daily activities might be a stronger surgical candidate than someone reporting severe pain who can still work, walk, and maintain independence.
Functional indicators surgeons assess:
- Walking distance before pain forces you to stop
- Ability to perform work-related tasks
- Sleep disruption from knee pain
- Dependency on walking aids or assistance
- Impact on social activities and mental wellbeing
According to the NICE joint replacement guidelines, shared decision-making requires discussing treatment options with patients and their families, including the potential benefits and risks of available procedures. This is where functional assessment becomes crucial—it provides the objective framework for that conversation.
The Conservative Treatment Threshold: What You Must Try First
Here is a statistic that might surprise you. The vast majority of patients initially presenting with knee problems will not require surgery. Conservative management works for many conditions—and most healthcare systems require evidence that you have genuinely tried these approaches before surgical options are considered.
Physiotherapy, weight management, activity modification, pain medication, injections. These are not obstacles placed in your path to delay inevitable surgery. They represent genuine treatment options that resolve symptoms for many patients. Surgeons need to know you have given them a proper chance.
I observed a case that illustrates this perfectly. Sarah, a 42-year-old recreational tennis player, arrived at consultation convinced she needed immediate ACL reconstruction following a partial tear. The surgeon recommended physiotherapy first. Sarah was disappointed—frustrated, even. Six months later, she had returned to tennis. Surgery avoided. Her initial assumption that surgery was the only option had been wrong.
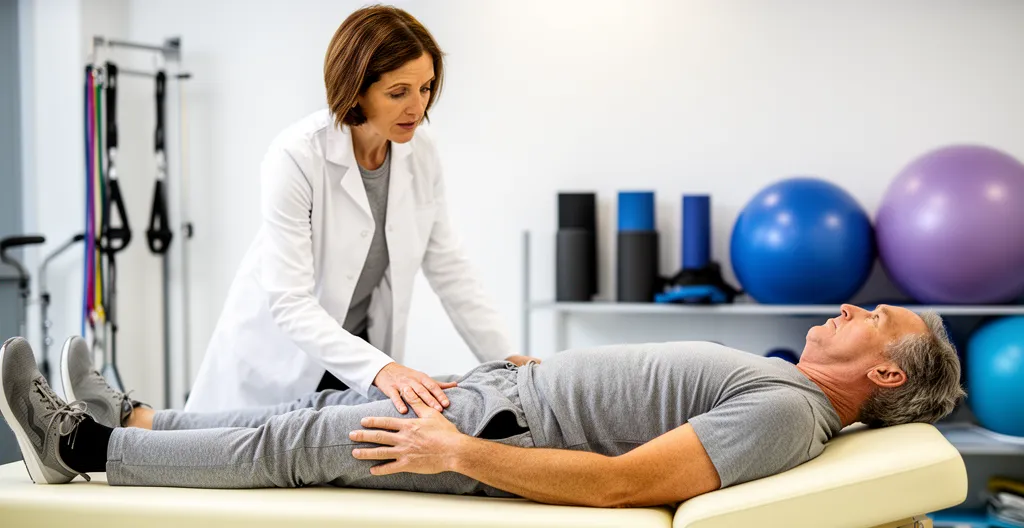
If you are exploring natural solutions for joint pain as part of your conservative management journey, you are taking the right approach. Documenting what you have tried—and honestly assessing how well it worked—prepares you for a more productive surgical consultation.
-
Initial consultation and clinical examination with orthopaedic specialist -
Imaging studies (MRI, X-ray) and results review -
Conservative treatment trial: physiotherapy, medication, lifestyle modification -
Follow-up assessment: response evaluation and treatment planning -
Surgical decision based on documented treatment response
The duration of conservative treatment varies by condition. Osteoarthritis management might span months to years. ACL rehabilitation programmes typically run twelve weeks before reassessment. What matters is demonstrating genuine engagement with these approaches—not simply waiting out a prescribed period while doing nothing.
Your Overall Health: The Surgical Risk Calculation
Frankly, this is where some difficult conversations happen. Your knee might be an excellent candidate for surgery. Your body might not be.
Every surgical procedure carries risk. Anaesthesia, infection, blood clots, poor wound healing. Certain health conditions amplify these risks significantly. Surgeons must weigh the potential benefit of surgery against the likelihood of complications—and sometimes that calculation does not favour proceeding.
The Canadian Orthopaedic Association obesity guidelines state clearly that body mass index is an imperfect measure of obesity and should not be used to inform surgical candidacy cut-offs. A holistic surgical and medical assessment should be undertaken to understand the risk-benefit profile of each individual patient. This represents a shift from older practices where rigid BMI thresholds sometimes excluded patients who might have benefited from surgery.
Health factors that may delay surgery: Uncontrolled diabetes significantly increases infection risk. Active smoking impairs wound healing and bone fusion. Severe cardiovascular disease raises anaesthetic concerns. These are not permanent barriers—they are modifiable factors. Optimising your health before surgery improves outcomes. Surgeons who recommend delaying for medical optimisation are protecting you, not dismissing you.
The ACR/AAHKS surgical timing guidelines conditionally recommend against delaying surgery solely to reach a target body mass index. They do recommend delay for nicotine cessation and improved glycaemic control in diabetic patients. The nuance matters. Some factors warrant delay. Others do not.
What I observe in clinical practice is that age alone rarely determines candidacy. Modern orthopaedic practice evaluates overall fitness rather than chronological age. An active 75-year-old with well-controlled health conditions might be a better surgical candidate than a sedentary 55-year-old with multiple unmanaged comorbidities.
Patient Expectations and Lifestyle Goals: The Often Overlooked Factor
This is the factor that rarely appears in medical textbooks but profoundly influences surgical outcomes. What do you actually expect from surgery? And are those expectations realistic?
Think of surgical candidacy like applying for a demanding job. Having the right qualifications (structural damage, failed conservative treatment) matters. But so does being the right fit—having goals that align with what the position actually offers. A knee replacement will not make you a marathon runner if you were never one before. ACL reconstruction does not guarantee return to elite sport. Arthroscopy cannot reverse advanced arthritis.
Research consistently shows that alignment between patient expectations and likely outcomes influences post-surgical satisfaction. Patients with realistic expectations report better outcomes—not because their surgical results differ, but because their assessment of success matches reality.
Surgeon’s perspective: Honestly, self-diagnosis from internet research rarely captures the full picture. A thorough clinical evaluation by a specialist who performs high volumes of knee surgery remains the gold standard for determining candidacy. No online tool can replace hands-on examination.
Understanding the link between chronic pain and inflammation can help you appreciate why surgery targets mechanical problems but may not eliminate all discomfort. Your lifestyle goals—returning to sport, walking without pain, maintaining independence—should be explicitly discussed with your surgeon.
Before your surgical consultation: expectation alignment
- Write down your specific functional goals (activities you want to resume)
- List all conservative treatments tried and their duration
- Prepare questions about realistic post-surgical outcomes for your age and activity level
- Consider your commitment to rehabilitation (typically months of dedicated physiotherapy)
- Assess your support system for the recovery period
Psychological readiness matters too. Are you prepared for the rehabilitation commitment? Knee replacement recovery takes months. ACL reconstruction demands disciplined physiotherapy for nearly a year. Surgeons assess whether you understand this commitment—because the best surgical technique cannot compensate for poor rehabilitation compliance.
The next step for you
Surgical candidacy is not a simple yes-or-no question. It emerges from careful consideration of structural findings, functional impact, treatment history, overall health, and personal goals. Understanding these factors transforms your consultation from a passive experience into an active partnership.
My recommendation? Document your journey before your appointment. Keep a record of treatments tried, activities affected, and goals desired. This information makes the surgeon’s assessment more efficient and more accurate.
Rather than asking whether you need surgery, perhaps the better question is: what would surgery need to achieve for you to consider it worthwhile? Start there, and you arrive at your consultation ready for a genuinely productive conversation about your options.
Important considerations before your consultation
- These clinical factors are general evaluation criteria and may vary based on individual circumstances
- Each patient’s anatomy, medical history, and lifestyle require personalised assessment
- Only a qualified orthopaedic surgeon can determine surgical candidacy after proper examination
Your questions about surgical candidacy
Can I be too old for knee surgery?
Age alone is rarely a contraindication. Modern orthopaedic practice assesses overall fitness rather than chronological age. Patients in their eighties undergo successful knee replacements when their general health supports safe surgery and recovery. The key factors are cardiovascular fitness, ability to participate in rehabilitation, and realistic expectations about outcomes.
Does severe pain mean I definitely need surgery?
Pain severity alone does not determine surgical candidacy. Surgeons look for correlation between symptoms and structural damage visible on imaging. Severe pain with minimal structural findings might indicate conditions better treated non-surgically. Conversely, significant structural damage with moderate pain might warrant intervention to prevent further deterioration.
What if I have been told to lose weight before surgery?
Current guidelines increasingly recommend against rigid BMI cut-offs for surgical eligibility. While weight optimisation can reduce certain surgical risks, blanket delays for weight loss are being reconsidered. Discuss your specific situation with your surgeon—the decision should reflect your individual risk-benefit profile rather than arbitrary thresholds.
How long do I need to try physiotherapy before surgery is considered?
Duration varies by condition. Osteoarthritis management might span several months. ACL rehabilitation programmes typically require twelve weeks before reassessment. The key is genuine engagement with conservative treatment—completing prescribed exercises, attending sessions, modifying activities as recommended—rather than simply waiting out a prescribed period.
What happens if I am not a surgical candidate?
Being declined for surgery is not the end of treatment options. It often means conservative approaches have not been fully optimised, or that modifiable risk factors need addressing first. Injection therapies, advanced physiotherapy, bracing, activity modification, and weight management can significantly improve symptoms. Some patients become surgical candidates after optimising their health status.